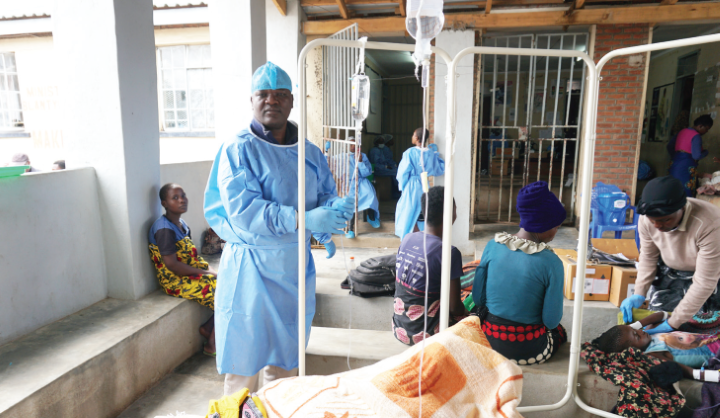
Malawi’s paralysing health crisis
She woke up weak and dizzy. While in the bathroom, Chrissie’s arms grew numb. She collapsed.
That was in 2016. Now, she recounts how a splitting headache suddenly paralysed her limbs.

“I couldn’t feel my left arm and leg. Before I knew it, I was down,” she says.
An hour later, she was on a sickbed at Queen Elizabeth Central Hospital (QECH) in Blantyre. Doctors diagnosed her with stroke.
She is lucky to have survived the interrupted flow of oxygen-rich blood to the brain
Haemorrhagic stroke, the commonest in Malawi and the rest of Africa, is a silent killer. It leads to the leaking of blood in the brain, following a ruptured blood vessel.
The incidence of stroke, like other non-communicable diseases (NCDs), does not only increase with age, but also a sedentary lifestyle and unhealthy diets.
Figures at QECH, one of four referral hospitals in the country, suggest a surge.
“The facility admits five stroke patients a week,” says Dr Laura Benjamin.
This means 140 cases in a year.
Nearby, Kachere Rehabilitation Centre assists stroke victims regain their speech, occupational wellbeing and mobility.
“The centre has 40 beds against an average of 50 patients on our waiting list. Nearly half of the patients we see here are suffering from stroke,” says physiotherapist Bester Kamakanda.
His schedule is usually tight.
Walking to his office, sights of stroke patients on wheelchairs flashed past.
“We only have 18 functional wheelchairs but just five are self–propelled—the type recommended by the World Health Organisation [WHO],” he said.
The self-driven wheelchairs help patients exercise on their own. They cost between K160 000 and K270 000 each.
A few private patients, who commute from home, pay K9 000 a day. Those admitted here get the service free.
According to Kamakanda, they often get discharged after three months to continue on a home-based programme.
“Over the past five years, the number of stroke patients coming for rehabilitation here has tripled,” he says.
WHO estimates that NCDs cause seven out of every 10 deaths globally. These chronic illnesses include diabetes, cancer and stroke.
By 2025, these diseases are projected to kill 120 million people, especially in low to middle income nations.
In Africa, for example, the number of people suffering from hypertension—the number one cause for stroke—was projected to jump from 80 million in 2000 to 150 million in 2025.
These diseases have common risk factors, including smoking, insufficient physical exercises, unhealthy diets and alcohol abuse.
Sustainable Development Goal (SDF)3.4 seeks to reduce by one third premature deaths caused by NCDs by 2030.
This calls for improved prevention and treatment.
The NCD Alliance is a network of civil society organisation pushing for a world where everyone has the opportunity for a healthy life, free from preventable suffering, stigma and death caused by NCDs.
It warns that without urgent, bold, coordinated and focused global action, the world might be “sleepwalking into a sick future”.
Like never before, there is need for a sense of urgency and political courage for action; scaling up of resources to match the burden and a sharpened focus on implementing what works.
Imbedded in the three-pronged agenda are calls for preventive efforts.
Among other things, health experts encourage the use of herbs, vinegar and lemon to flavour foods to reduce salt consumption salt, which causes hypertension.
Presently, NCDs hurt human health and economies.
The United Nations estimates that the world will lose $50 trillion due to NCDs by 2030. This is about four percent of the annual global gross domestic product (GDP).
“If not well managed, high blood pressure can also weaken arteries and make them more likely to burst. If the blood leaks in the brain, it will cause haemorrhagic stroke,” says Mwanza district health officer Dr Medson Matchaya.
For 51-year-old Chrissie, her condition has since robbed her of her job.
“I used to help my husband fend for our four children. Not any longer,” says the nurse, pausing as she confronts the painful reality of how stroke has wrecked her health, livelihood and independence. “After over a year of illness, my contract was terminated.”