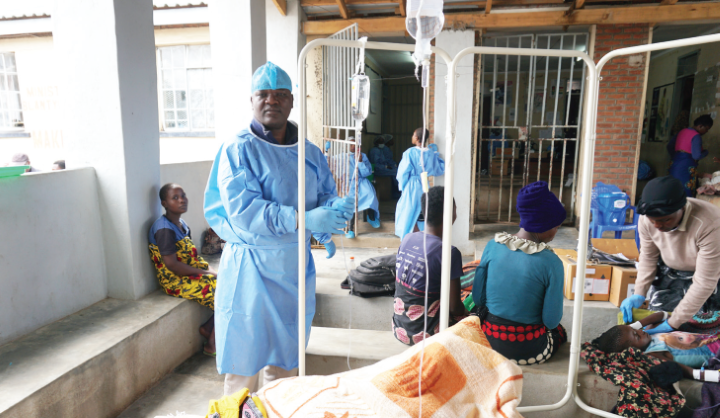
Bleeding is number one killer of mothers
 The widely opened wooden door of the health centre brought a sigh of relief to 28-year-old Nangozo (not real name). She had delivered a baby girl at home.
The widely opened wooden door of the health centre brought a sigh of relief to 28-year-old Nangozo (not real name). She had delivered a baby girl at home.
Wrapped in a pink shawl, a traditional colour for girls, the newborn seemed oblivious to reality as she lay beside her mother in the donkey cart that was being driven by her father in the company of three relatives.
Nangozo was battling for her life during the five hour journey to Chimalizeni Health Centre (not real name) but kept her strength up for her daughter’s sake as she struggled to breast-feed it at two hourly intervals. But as the sun closed in on them, she became too weak from the loss of blood.
She and the four kinsmen braved the heat to get to the hospital for further treatment after delivering the baby. Theirs was a hope for the well being of the mother of four who had previously delivered three boys and was desperately longing for a girl.
Two hours upon arriving at the hospital, she continued bleeding as she lay on a mattress on the floor as personnel attempted in vain to arrest the situation.
At exactly 7:30 pm, Nangozo was pronounced dead as the distant cries of her infant rang in the ears of those that surrounded her bed in tears. The long trek had all been in vain. So much for the dream of a girl that Nangozo will never know.
Her condition is described clinically as postpartum haemorrhage (PPH). According to wikipedia.org, it is the loss of greater than 500ml of blood following vaginal delivery or 1000ml of blood following Caesarean section.
It says that PPH is the most common cause of perinatal maternal death in the developed world and is a major cause of maternal morbidity worldwide.
The East, Central and Southern Africa Health Community (ECSA-HC) says postpartum haemorrhage is the number one killer of mothers in its eight member region comprising Malawi, Kenya, Tanzania, Uganda, Lesotho, Mauritius, Swaziland, Zambia and Zimbabwe.
Family and reproductive health manager for ECSA, Dr. Odongo Odiyo, told journalists from the region last week that haemorrhage causes 36 percent of maternal mortality seconded by hypertension and indirect causes at 18 percent; other direct causes at 11 percent; unsafe abortion at 9 percent and sepsis at 8 percent.
Odiyo said deaths of mothers continue to occur in spite of global and regional commitments to deal with the situation.
He cited, among others, the safe motherhood conference in Nairobi in 1978; the 1994 International Conference on Population and Development (ICRD) in Cairo; the Millennium Development Goals (MDGs) in 2000; Abuja Declaration in 2001, Maputo Plan of Action in 2006; Ouagadougou in 2008; the Campaign to Accelerate Maternal Mortality in Africa (CARMMA) in 2009 and the ECSA health ministers’ resolutions in 1999 to 2009.
To worsen the situation, Odiyo said an assessment conducted by ECSA and its partners in 2007 revealed that only 5.7 percent of health workers in study countries of Uganda, Tanzania and Ethiopia were correctly using the Active Management of Third Stage Labour (AMTSL), a key component to stopping excessive bleeding in mothers.
Said Odiyo: “This finding was due to the fact that the World Health Organisation (WHO) guidelines on AMTSL were not adhered to. There is need to review the guidelines and to close the gap skills and knowledge in management of PPHâ€.
As a means of managing PPH within the ECSA region, Odiyo said health ministers held a dialogue in 2008 on prioritising AMTSL practice in the region which resulted in the passing of a resolution on maternal and child health, reproductive health and family planning.
The resolution urged member states to institutionalise the practice of AMTSL in all health facilities providing maternity care, directed ECSA secretariat to support this process which in turn supported the review of AMTSL guidelines in 2009/2010 with the support of its working partners.
“The revised guideline was disseminated in Tanzania and Ethiopia in 2010.
To date, the two countries have rolled out and scaled up the use of the guidelines in several districts. ECSA also supported the same in Uganda in 2011 and prepare job aids for AMTSL practice,†said Odiyo.
He further said a review of policies by member states was undertaken in 2010 and although all countries were found to have relevant policies, they had problems in their implementation because of inadequate human resource skills in lower facilities, in referral of complicated cases, commodity stock outs and difficulty in the storage of oxytocin; a hormone that helps relax and reduce blood pressure.
He said WHO is currently concluding a multi-country study on the use of misoprostol, a drug which has now been approved for the management of PPH.
Odiyo said AMTSL helps reduce PPH through the administration of uterotonic drugs such as oxytocin and ergometrine; controlled cord traction and uterine massage.