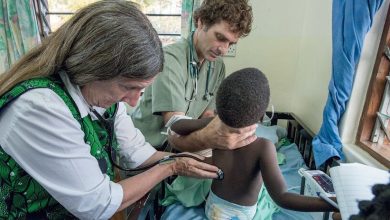
Speeding between life and death
The jagged road from Chitipa to Mzuzu is long. Winding past hills and valleys for seven hours on cratered tarmac, ambulances seldom start off with a full tank.
The Northern C orridor is rough for kidney disease patients from the northernmost district.

A patient renamed Yohane Tembo, 42, has not walked freely for weeks. His legs swell. His breathing is shallow. His bones feel older.
Doctors at Chitipa District Hospital suspect his kidneys have collapsed, but he is awaiting fuel for an ambulance to take him to Mzuzu Central Hospital for someone to confirm that he needs dialysis at least twice a week to live longer.
His story is familiar in the North.
The six-district region—home to two million people—has no dialysis machines to filter waste salts from patients’ blood when kidneys fail and urine stops.
Chronic kidney disease is on the rise in the country, where over 400 patients are on treatment—up from 300 last year.
“The district recorded two cases in 2022–23 fiscal year, four the following year and six between April 2024 and March this year. More may not be officially recorded,” says Chitipa director of health services Jellings Kasondo.
The medical doctor says the surge is fuelled by untreated hypertension, diabetes and increasing use of herbal concoctions with unknown chemical contents.
“People believe in what they know, but their kidneys can’t process it. By the time we see them, it’s often too late.”
Like all 28 districts, Chitipa has no dialysis machine. When kidneys collapse, patients have to travel 700 kilometres to Kamuzu Central Hospital (KCH) in Lilongwe, which has 10.
Every diagnosis triggers a slow chain reaction, from confirmation at Mzuzu Central Hospital (MCH) to a 370-kilometre ambulance trip that takes at least seven hours.
“Each round trip [to Mzuzu] burns fuel worth about K275 000. With allowances for drivers and clinicians, the cost exceeds K500 000. The district doesn’t usually budget for such referrals, but we can’t just leave patients to die,” says Kasondo.
The costly travels exposes the price of scanty investment in kidney health.
As patients pour in from six northern districts, the waiting list for the scarce ambulances from MCH, the region’s largest hospital, to KCH keeps lengthening.
Construction plant and bumpy diversions frequently slow the dreaded medical trips on the rutted M1, currently under rehabilitation.
The patients in agony arrive at KCH weak and battered, with breathing difficulties.
Last year, MCH admitted 69 chronic kidney disease patients in nine months, but some are still waiting for their dialysis debut.
MCH spokesperson Arnold Kayira says many make out-of-pocket payments for the urgent trips just to keep up with dialysis schedules.
“The conditions often worsen as they wait to start dialysis,” he says.
Some families sell their prized assets—land, crop harvests, livestock, vehicles and homes—to make the trip. Others get trapped in debt, refusing to give up.
Several reach KCH, only to be sent back to wait for a turn as the dialysis machines remain too few.
“There are no guarantees, only fatigue and frustration,” says Mrs. W. Chafulumira, from Karonga District.
She was diagnosed with kidney failure at the age of 19.
Chafulumira narrates: “There was no place to stay, so I took shelter in the hospital premise for 11 months.
“I was just about to start university, but I was uprooted from my parents’ home. Now I’m stuck in Lilongwe.”
This shows how gaps in kidney health dim futures and split families.
Chafulumira says the long travels in search of dialysis do not only make patients and their caregivers poorer, but also cut patients’ lifespans.
She undergoes the five-hour blood-cleaning process on Mondays and Thursdays.
The patient fears to return to the North.
“I’ve seen others go back after treatment, only to relapse and die,” she says.
Chafulumira asks government to procure dialysis machines for strategic hospitals like Karonga for districts at the northern tip and Mzuzu for the rest of the underserved region.
Kayira says the Ministry of Health is in the final stages of establishing a dialysis unit at MCH.
According to the publicist, there is a dedicated committee coordinating the cause.
Kayira states: “The procurement process of six machines is complete; we’re now at the intention-to-award stage. Supplies are in, renovations are underway and core specialists ready. Soon, our nurses and clinicians will travel to KCH to learn how their peers manage the machines.”
He terms this a game changer, envisioning patients getting treatment closer to home, on time and without financial hardship.
“The dialysis unit will not only save lives, but also patients’ income,” says Kayira.
Malawi Health Equity Network (Mhen) executive director George Jobe says the ongoing procurement of MCH dialysis machine is encouraging.
He states: “However, our wish is that the machines should be available for a cluster of districts since central hospitals are far from some districts.
“However, he warns that blood-cleaning machines alone won’t save lives. We need to talk about prevention too. Many kidney cases are avoidable. Simple habits, like drinking enough water, can make a difference. People need awareness,” he says.
To Chafulumira, the dawn of dialysis in Mzuzu signals “what healthcare should be: close, dignifying and valuing every life”.
“I weep for patients who died at home, on the road or while waiting for a turn,” she says.
“This had to end,” she says.