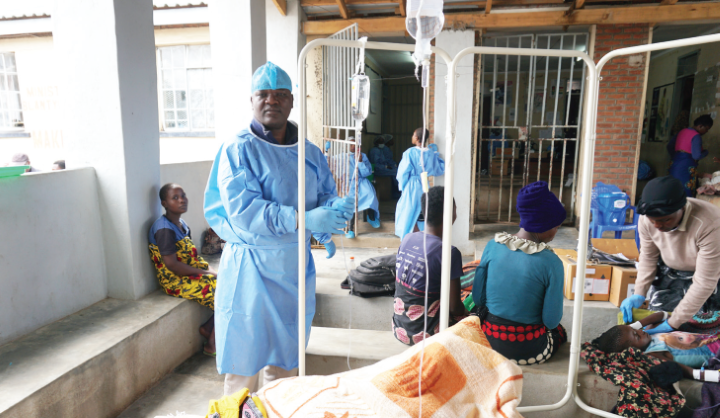
When a referral hospital operates without an operating theatre
From a distance, Chintheche Rural Hospital, looks like any other hospital.
Painted in white, no one can miss the cleanliness and orderliness at this facility, which lies on the beautiful shores of Lake Malawi, 40 kilometres south of Nkhata Bay.

However, the hospital, which caters for 25 000 people, does not have a functional operating theatre. A chat with hospital authorities singles out pregnant women as the most affected group.
“Women are dying in childbirth. It is sad to look at pregnant women in pain, knowing there is nothing you can do but refer them to Nkhata Bay District Hospital because we do not do surgical operations here,” Kayaya Thera, the district’s nursing officer, explains.
Thera cites an example of a 27-year-old woman, referred to Chintheche Hospital from Liwuzi Health Centre, who died due to post-partum haemorrhage.
“The woman was supposed to travel 40 kilometres to Nkhata Bay District Hospital for an operation, but unfortunately she did not make it, she died on arrival at the hospital,” she says.
Nkhata Bay is not the only place where women are dying as a result of pregnancy and childbirth complications. Recent studies indicate that Malawi registers 645 maternal deaths per 100 000 live births.
Although the country’s maternal death rate has declined by 53 percent between 1990 and 2013, the rate is still high. Last year alone, maternal deaths were estimated at 3400, with most deaths in rural and hard-to-reach areas.
Pregnant women who visit Chintheche Rural Hospital brace for hard times in case they have complications and have to be ferried to the district hospital for a Caesarean section.
Chintheche Hospital incharge Greyson Kumwenda said the absence of an operating room puts pregnant women at great risk.
“With pregnant women, you never know when you might have a case with complications. Our lack of an operating theatre is worsening pregnancy and childbirth related deaths,” Kumwenda says.
A 2009 Amnesty International report rates Malawi as one of the 14 countries with the highest maternal mortality ratios globally. The report says the main causes of maternal deaths in the country are puerperal sepsis, obstructed labour, ruptured uterus, haemorrhage, eclampsia and unsafe abortion.
It is estimated that approximately 74 percent of maternal deaths could be prevented if all women had access to services which would prevent or treat such pregnancy and childbirth related complications.
The referral hospital has a structure meant to house the operating theatre whose construction stopped due to lack of funding.
Kumwenda says for the theatre to be operational, it needs operating lights, beds, tables, a corridor connecting the old and new maternity wing and a plumbing system.
“The project was supposed to be completed by March 31 this year, however, because of lack of funding; we are not sure when it will be finalised,” he says.
According to the hospital incharge, the facility has on average 120 natural deliveries a month and about 15 Caesarean section cases which they refer to the district hospital.
“Without a functional operating theatre, safe motherhood is a far-fetched dream here. We have the expertise, but we lack the necessary equipment to do the job,” Thera explains with deep sadness.
Touched by the situation, the Mzuzu Lions Club promised to source funding to assist the hospital.
“Some friends of Mzuzu Lions Club from the UK have already offered surgical equipment like operating beds and lamps, the only challenge is shipping,” Lions past district governor Faisal Karim states.
Some surgical equipment that the lions club donated to the hospital in the past is gathering dust in the hospital’s warehouse awaiting the completion of the operating room.