Kidney crisis deepens
Recently, Kamuzu Central Hospital (KCH) in Lilongwe shuttled a busload of its kidney disease patients to Mwaiwathu Private Hospital in Blantyre following a stutter in the government-owned dialysis machines.
The breakdown in artificial kidneys left the patients who need the blood-cleaning service twice or thrice a week bearing extra costs.
The worst hit were those without friends and relatives to accommodate them in the receiving city, and some lost their lives because they could not afford routine care away from home.
This highlights a neglected gap in the healthcare system. The nation of about 22 million people has only two public health facilities—KCH and Queen Elizabeth Central Hospital (QECH) in Blantyre—offering the service to such patients while awaiting kidney transplants.
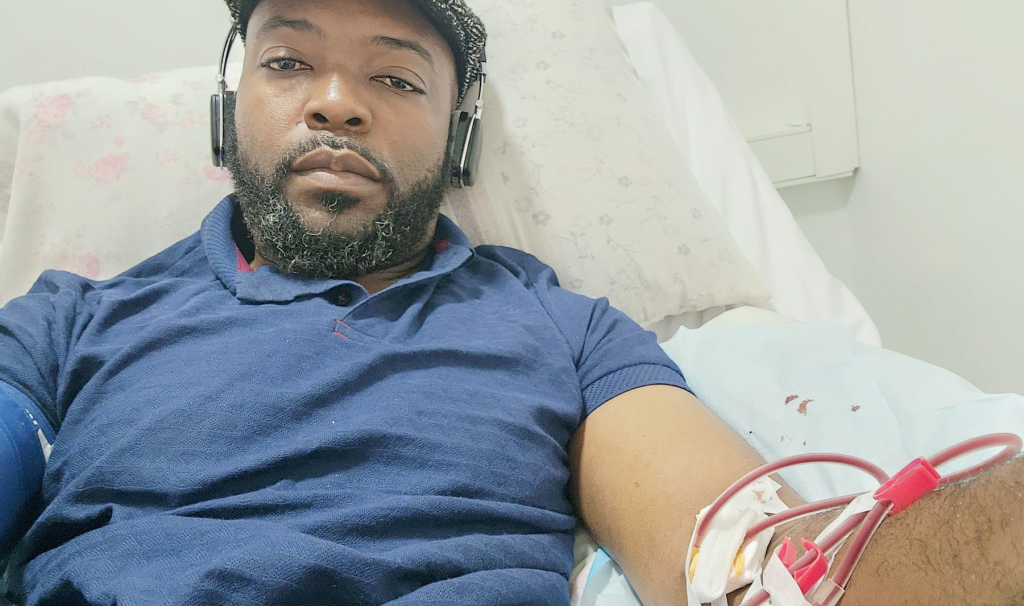
Costly ommission
Quirky, there is no single dialysis for the entire Northern Region, home to about three million Malawians. The Ministry of Health promised to open a dialysis centre at Mzuzu Central Hospital last year, but the machines that were said to be under installation remain unavailable to those who need them most.
Meanwhile, northerners who require dialysis still travel to Lilongwe, where only KCH and Partners in Hope Private Hospital offer the service.
This leaves dozens dying of the treatable conditions because of low investment in kidney care, treatment and support.
Across the country, those who cannot afford the long hospital trips and appointments with private clinics that cost about K700 000 a week die while waiting for a turn in overcrowded public dialysis sites.
Unfortunately, a slot for a new entrant only opens when death occurs and many die waiting.
The Nation exposed the suffering of patients with chronic kidney disease, asking why only two out of over 500 public healthcare facilities nationwide provide artificial kidneys for people whose pair has collapsed.
The assignment exposed a health system struggling to keep pace with a silent but costly epidemic that leaves many a medical bill away from poverty, except those in power who frequently fly beyond the borders for better care on the suffering taxpayer’s bill.
Health authorities say patients on treatment surged from 300 to over 400 in 2025, but more remained undetected and untreated due to low investment.
Many reach hospitals too late for any care beyond dialysis.
“Most of our patients come when the damage is already irreversible,” says QECH kidney specialist Dr Khumbo Chisale. “If we identified them early, many would never reach dialysis.”
Delays in diagnosing and treating hypertension and diabetes fuel kidney conditions that trigger a fierce scramble for dialysis machines.
Rural health facilities lack basic equipment, allowing warning signs to go unnoticed.
Further, long travels to central hospitals continue to define who lives longer.
Patients from the North and 20 districts outside Lilongwe and Blantyre pay a huge cost to access kidney support.
Some miss appointments when they cannot afford the costly hospital trips and others sleep on hospital verandas while waiting for dialysis sessions.
“I spend more time on the road than at home. If I miss one session, my body feels it immediately,” says Mzuzu-based Peter Gondwe.
Vitani Kamanga relocated from Chitipa to Lilongwe to access the blood-cleaning machines at KCH.
“My wife and children followed me to Lilongwe, but life has not been easy. Others cannot afford the long trip,” he states.
Dialysis is supposed to be a lifeline, but it has become a burden as government hospitals struggle with limited machines, costly supplies, frequent breakdowns and fewer staff. Private clinics are unaffordable to many Malawians, who no longer work despite mounting medical bills.
Maria Nkhoma sold her maize field to keep her husband on dialysis in Blantyre.
“I paid for three months,” she said. “Now we don’t know what comes next.”
To healthcare officials, dialysis is no cure, but a life-prolonging service, as the country does not offer kidney transplantation.
Government and medical insurers report growing cost of subsidies and overseas referrals.
A lucky few who can afford transplantation, the ultimate treatment, seek surgery abroad, while the rest rely on dialysis.
“The absence of transplant services keeps us stuck in an expensive cycle,” says Dr Beston Chisamile from the Ministry of Health. “Dialysis keeps people alive, but it does not restore productivity.”
This is a tale of neglected inequalities at a time when ‘quality health for all’ has become a slogan of the global and national agenda for universal health coverage.
Poor patients drop out of treatment first. Rural patients—whose quality of life is the constitutional yardstick of government’s policies, according to Section 13—travel farther.
As authorities invest elsewhere, kidney issues silently break families, breadwinners lose jobs, children quit school and employers lament falling productivity and rising funeral expenses amid preventable deaths.
Apart from the sluggish establishment of a dialysis unit in Mzuzu, the government has recruited kidney doctor Mercy Mkandawire to establish a transplantation centre, but timelines remain unclear.
One of Malawi’s four nephrologists, she helped establish Namibia’s transplant programme.
Prevention matters
However, prevention also gained urgency. Authorities acknowledged that unchecked high blood pressure. diabetes, alcohol abuse, high salt diets and unregulated herbal medicines are driving kidney failure.
“We must stop meeting patients at the last stage. The fight against kidney disease starts in villages and health centres, not dialysis units,” says Chisamile.
As Malawi enters 2026, chronic kidney disease stands as both a medical emergency and a governance test.
Patients continue to wait on roads, in wards and beside machines, dying of treatable conditions as the rich and famous get the service across the borders.




