Life savers take disrupted services to disaster zones
It is 9am and a forming crowd perching in tree shades at Dulasanje Health Post in Chikwawa is waiting for healthcare workers and supplies coming to their hilly community.
On arrival, the healthcare team first offers a public talk on available services, including family planning, treatment for common diseases, HIV testing and treatment as well as routine immunisation for children aged below five.
“If you take antiretroviral drugs consistently, your viral load drops to undetectable levels, so you can enjoy healthy and productive lives with a suppressed risk of transmitting the virus that causes Aids to newborn and breastfeeding babies and sexual partners,” says a nurse leading the team.
This sounds good for a 38-year-old businessperson disguised as Mercy William. She was diagnosed with the virus in 2017 when she took her 11-year-old daughter to their nearest clinic.
The devastating Cyclone Freddy that hit southern Malawi in March this year battered Mercy’s house to rubble, forcing her to flee to a congested camp with her family. She feels lucky that the four-day rainstorm struck just days after she had replenished the drugs she takes daily around 6am.
“Just before the two walls of my house collapsed, I had enough pills for three months. I grabbed the bottle containing the antiretroviral [ARV] drugs, three skirts and two blouses, then fled to a nearby primary school where I camped for three months with my family,” she says.
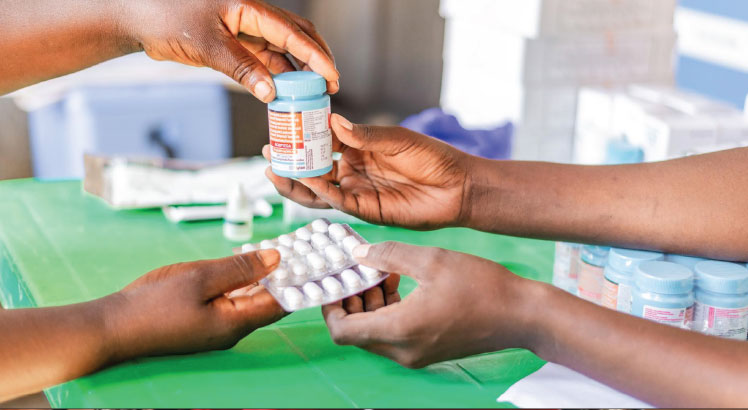
“However, life in the congested camp was unbearable for people on antiretroviral treatment as I had no food, no money and no privacy; I couldn’t take the drug with persistent food insecurity, uncertainties caused by displacement and all eyes on me.”
Mercy often woke up before daybreak, taking her bucket and discreetly swallowing the daily pill on the way to a communal water pump.
Besides, her campmates, whose ARVs and cards were washed away in the flooded zones, run the risk of quitting HIV treatment.
This increases the danger of developing deadly resistance to the drugs and dying from diseases that thrive on low body immunity.
“It took a month for teams from Chikwawa district health office to start coming to our aid. They used to bring essential medicines, including ARVs,” Mercy recalls.
The mobile clinics supported by Unicef, in conjunction with Save the Children, helped bring integrated life-saving services closer to people who needed them.
The initiative is funded by the United Nations’ Central Emergency Response Fund and Bill and Melinda Gates Foundation to deliver timely and reliable humanitarian assistance to populations affected by natural disasters.
Mercy explains: “The mobile clinics were timely. Having lost everything to the tragedy, I couldn’t afford a K5 000 return trip to Mfera Health Centre downhill.
“Due to financial constraints, most of my neighbours used to walk six kilometres to Madziabango clinic, but I preferred getting my antiretroviral drugs from Chikwawa District Hospital to avoid stigma.
“The mobile clinic became handy because I could no longer afford the two-way medical trip worth K6 000, half the profit I was making from selling boiled meat before the business was disrupted by displacement.”
The clinic on the move propels national efforts to ensure everyone gets the health services they want close to where they live without experiencing any hardship, including long walks and financial burdens.
Malawi has embraced the universal health coverage policy to ensure everyone accesses health services within five kilometres.
“The mobile clinic has saved the money and time once spent travelling to Chikwawa District Hospital. The savings are enough to buy nutritious food for my child and I can use the time to travel to Mpemba in Blantyre, where I order meat for sale,” she recounts.
The meat business, coupled with samosa sales, generate K12 000 to K15 000 a day, says Mercy.
Kingsley Khokho, a health surveillance assistant at Dulasanje Health Post under Mfera Health Centre, says the mobile clinics bring multiple healthcare services closer to the displaced population.
He said: “The mobile clinics put various health services under one roof, making it convenient for people in camps and affected zones. This was important during the emergency response because people on HIV treatment had lost their drugs, and homes where they felt safe to store and take the drugs.
“Now they were living in overcrowded spaces where all eyes were on them and food was scarce, making it risky for one to take ARVs on an empty stomach.”
Nearly 220 houses collapsed in villages surrounding Dulasanje Health Post.
This gives a glimpse of the devastation the Department of Disaster Management Affairs terms the worst natural disaster since 2000.
Dodma’s post-disaster needs assessment report shows that the cyclone affected more than 2.2 million people, leaving 659 278 displaced, 679 dead and 530 missing.
During the mobile clinic, Patricia Felix brought her one-year-old daughter Yankho, who was found with malaria after experiencing high fever, vomiting and breathing difficulty.
The woman also wanted a family planning injection she has been taking discretely since February this year. The jab helps her prevent unintended pregnancies for six months.
“I’m happy that we aren’t wasting hours or enduring long travels to get the healthcare services we need. This has made life easier and many people are coming to benefit from the outreach clinic,” said the mother of three daughters, aged and to 11.




