Cholera among us again
Cholera has become a seasonal killer in one of Blantyre City’s clustered settlements, marked with blocked drains, leaking pit latrines, soiled diapers discarded in open spaces, pit latrines emptied into waterways and streams turned into dumpsites.
In the populous Chilomoni Township, foul-smelling wastewater snakes between crowded homesteads on the way to the nearest stream.

a previous outbreak.
For resident Aida George, 26, cholera, which has claimed a life in Chilomoni, hit days after drawing water from a neighbour’s shallow well.
“The water looked clear, but…,” she stutters to a pause in an interview at her home in Mulunguzi area.
George was cooking supper for her family of four when vomiting and diarrhoea hit her.
Neighbours carried her on a bicycle to Chilomoni Health Centre cholera treatment camp, where she was discharged after four days.
“I was weak and severely dehydrated,” she recalls. “I hastated to seek treatment because the diarrhoea was slow.”
In the next bed lay John Chikwelekwese, 48, a Michiru Mountain conservation volunteer. “The disease took me by surprise as I was waiting for supper after a hectic day of guarding the plundered mountain and doing piecework to feed my family,” he narrates.
He recalls that the diarrhoeal disease hit him around 3am.
Chilomoni has become a cholera hotspot in Blantyre, with the treatment camp receiving over a dozen of cases from Mulunguzi.
Bucket line the floor. Chlorines hung in the air. Caregivers moved from bed to bed, hanging IV drips and providing other life-saving services.
“I feared death,” says George. “I thought of my two children. Who would cook and care for them if I die?”
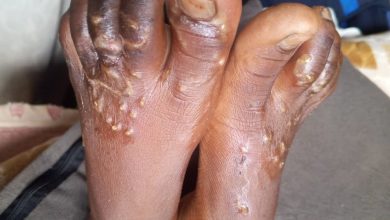
Cholera kills within hours if not treated on time.
Chikwelekwese says the disease, which is prevented through safe water, sanitation and hygiene, reduces an adult to a child.
In Mulunguzi settlement, overflowing pit latrines drip into gullies and streams where children play.
The community drinks water from the contaminated streams as taps are far apart and frequently run dry.
“We are at risk because we live on top of our own waste,” says George.
Her family shares a dilapidated pit latrine with seven other households, comprising over 20 people. Green fries commute between the latrine and foodstuffs, landing on utensils drying in the sun.
“Our lives are in danger, but where can we rent cheaper houses in the city?” she asks.
Chikwelekwese, a breadwinner for a family of eight, says the informal settlements “eats their own waste”.
“Only God protects us. We have no land for latrines, no running water, no toilets and no say,” he said.
George now boils drinking water to kill germs.
She says charcoal and firewood is expensive, “but life is precious”.
Similarly, Chikwelekwese carries treated water and food to work “to avoid street food” amid low access to clean water, sanitation and hygiene.
In the narrow alleys of Blantyre’s sewage-infested slums, the new cholera outbreak evokes memories of Malawi’s deadliest spate which claimed about 1 700 lives from over 55 000 patients between 2022 and 2023.
For them, the public health crisis is a story of poverty and inequality that disadvantages people on the margins.
Not everybody walked out of the cholera ward alive.
Agnes Majawa mourns her husband, an energetic young man who died within a day of falling ill.
She recounts: “He was cheerful when he arrived home from piecework in the city, but the situation changed fast. By night, he was vomiting uncontrollably, we took him to the hospital where he was pronounced dead after receiving seven drips.”
“Since his death, the home has grown quieter, with little to smile about. Our children ask when their father is coming back and the truth hurts.”
In a township where slimy water runs past doorsteps, she has learned that cholera can be devastating.
Edina Kayemeza, a volunteer who supports community health workers to stop the outbreak, believes low income levels cost lives.
“As community volunteers, we go door-to-door, promoting water treatment, sanitation and hygiene. But without adequate resources, such health talks are just noises. People here need clean water and clean latrines. Otherwise, we will die here,” she laments.
Village head Bayoli of Mulunguzi has signed letters for the sick, helped carry neighbours to the nearest clinic and consoled bereaved families.
“When cholera comes, it does not knock on the door. It enters our homes through unclean water and poor waste management. As a leader, I can encourage people to boil water and uphold sanitation, but I cannot give them running water, toilets and other sanitation facilities.”
According to health surveillance assistant Maggie Baluwa, Chilomoni alone registered 24 cases with one death.
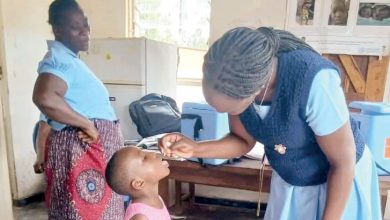
“Following the death, we administered oral cholera vaccines to about 98 percent in the township. People were terrified, so they queued for the vaccine. Resistance was almost zero,” she says.
Lillian Mwale says she queued for the vaccine because “this is the only way we can protect ourselves alongside insisting on safe water, sanitation and hygiene.”
The Ministry of Health and Sanitation reports that Blantyre District accounts for nearly half –30—of the 58 confirmed cholera cases nationwide.
In an interview, Blantyre district director of health and social services Gift Kawalazira blamed poor hygiene practices and low access to safe water for the outbreak.