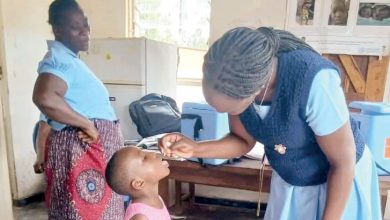
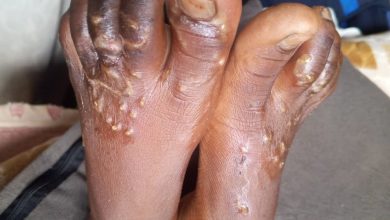
Climate shocks fuel cholera
In Nathenje, on the outskirts of Lilongwe District, 31-year-old Lezina Aaron is still struggling to recover from the shock of losing two children to cholera within a week in 2023.
After giving birth to her second child on January 7, Aaron and her newborn were admitted to Nathenje Health Centre, where the baby contracted cholera. At the same time, her seven-year-old son fell ill with the disease at home.

Her condition was critical. Placed on nearly 24 drips, she was too weak to breastfeed, even as her newborn desperately needed it.
“When I regained some strength, the doctor came to my room to break the news,” she recalls. “He told me my seven-year-old son had died of cholera. I couldn’t even attend his funeral.”
Days later, her newborn—who had been referred to Bwaila Hospital in Lilongwe—also died.
Aaron’s story reflects the growing human cost of climate-driven health crises, as floods, droughts and rising temperatures accelerate the spread of waterborne diseases such as cholera across southern Africa.
The climate–health link has gained global attention, including at the 30th UN Climate Change Conference (CoP30) in Belém, Brazil, where leaders warned that climate change is reshaping disease patterns.
The Belém Health Action Plan calls for stronger surveillance and evidence-based responses to climate-sensitive diseases.
For Malawi, which faces recurrent cholera outbreaks during flooding and heavy rains, the discussions reinforced the need to link climate adaptation with improved water, sanitation and hygiene (Wash) systems.
Overwhelmed
During the 2023 outbreak, hundreds of people died nationwide. Nathenje alone recorded 601 cholera cases and 41 deaths, with women the most affected.
Facility in-charge at Nathenje Health Centre, Mary Lujere, says the outbreak exposed serious gaps in the health system.
“It was our first time experiencing such a severe outbreak. We lacked equipment, supplies and capacity,” she says. “Many cases could not be managed effectively.”
In response, the facility began screening patients presenting with cholera-like symptoms, given the community’s limited access to safe water.
A 2024 Ministry of Health and Sanitation study shows that Malawi’s most severe cholera outbreak occurred in 2022/2023, with more than 53 000 cases and 1 586 deaths. Poor Wash conditions, worsened by extreme weather events, were identified as the main drivers.
Cyclones Idai, Anna, Gombe and Freddy—experienced within five years—damaged health facilities and water infrastructure, increasing cholera risk in already vulnerable communities.
Women’s burden
Women are disproportionately affected—not only as patients but also as caregivers.
In Nathenje, group village head Margret Paulo became her mother’s primary caregiver during the outbreak. Caring for her until her death disrupted both her leadership duties and livelihood.
“I could not do business or carry out my responsibilities,” says Paulo, whose fish-selling business collapsed during that period.
In Phalombe District, climate shocks further compounded the crisis. Cyclone Freddy washed away Nkhulambe Health Centre forcing health services to operate from temporary tents donated by Médecins Sans Frontières (MSF).
Senior Chief Nkhulambe, born James Andrew Kambanje, says poor Wash conditions and damaged infrastructure left communities exposed.
“At first, people did not understand climate change or its link to health,” he says. “But when cholera cases started rising, they understood its impact.”
In 2023, some 17 people fell sick in his area; only six survived. Pregnant women were forced to walk long distances to seek care, often relying on unsafe water, while children became increasingly vulnerable as access to treatment and vaccines declined.
“All we want is the hospital, which is still under construction,” Kambanje says, warning that recurring floods may drive health workers away if lasting solutions are not put in place.
Closing the gaps
WaterAid country director Peter Phiri says climate extremes reduce access to safe water, increasing cholera risk. Partners are supporting emergency Wash interventions and community awareness.
According to the Ministry of Health and Sanitation, these interventions and household chlorine distribution have helped reduce cases, with current figures being far lower than during the peak of the 2023 outbreak.
However, assessments show that while Malawi recognises the link between climate change and cholera, translating policy commitments into climate-resilient Wash infrastructure remains unfinished work.
As Malawi aligns its development path with Africa’s Vision 2063, treating cholera as a climate challenge—rather than a recurring emergency—will determine whether the country can protect its most vulnerable communities in an increasingly unpredictable future.
This story was produced with support from IDRC and Mesha.