Caregivers learn from every new born death
In Malawi, every child who dies in the first 28 days is a bittersweet learning point.
When a newborn cannot survive the critical month, an inquiry must begin with role players detailing what they did or failed to do to prevent the tragedy.
The mandatory briefings are part of neonatal death audits that help close the gaps On how hospital staff care for fragile babies.
“When we get the reports, we meet to analyse the cause of death and isolate modifiable factors that call for urgent or long-term interventions. We draw action plans to ensure no life is lost needlessly,” says nursing officer Hellen Mwafulirwa.
The nurse coordinates neonatal care at Chikwawa District Hospital and 25 rural health facilities that help women deliver safely.
“Every death calls for an audit. Within 72 hours or three days, the clinician is supposed to certify the death, fill neonatal registration forms and notify the team of the probable cause,” she says.
The committee is supposed to meet every Tuesday and Thursday for the stock-take.
However, neonatal death audits in Chikwawa suddenly stuttered in January 2025 when the US Agency for International Development (USAid) stopped funding some of its programmes.
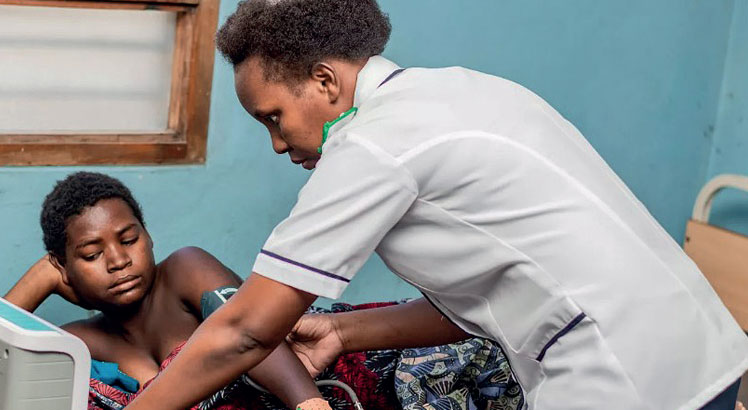
blood pressure. l Unicef Malawi
The committee resumed three months later with support from Unicef through the Umoyo Wathu Health Systems Strengthening project funded by the UK’s Foreign, Commonwealth and Development Office.
Mwafulirwa recounts: “Unicef intervened at the right time. The district recorded 75 deaths in three months—31 in January, 24 in February and 20 in March. With little motivation, members of the neonatal death audit committee kept skipping meetings and giving excuses.
“The support helped us scrutinise 60 percent of these deaths between April and June, which helped us to learn and almost halve neonatal deaths from 24 percent to 13 percent. This is a big improvement.”
Chikwawa District Health Office targets reducing newborn deaths to eight percent by March 2026, beating the national goal of 12 percent by 2030.
The audits exposed gaps in the treatment of premature and critically ill babies requiring artificial oxygen, persuading Unicef to support Chikwawa with six oxygen concentrators.
As part of the recommendations from the audits, health authorities placed oxygen cylinders in some ambulances for safe referrals of critical patients.
“Not all health facilities have oxygen concentrators and cylinders, but most patients now arrive in a stable condition,” Mwafulirwa states.
As newborn care improves, Mwafulirwa’s team conduct regular spot checks to ensure babies get recommended medication and oxygen doses.
With attention to detail, the number of children who experience breathing difficulty after swallowing fluids during birth is decreasing.
The caregivers also advise mothers to breastfeed the baby when certified fit and check preterm babies’ blood sugar levels every two hours.
“Reliable care and support build public confidence in the healthcare system. These days, many women come to deliver here,” Mwafulirwa says.
Lucia Stewart, aged 25, delivered her second-born son, Yonas, at St Montfort Mission Hospital in the sugar-producing rural town of Nchalo in CHikwawa District on 24 November 2025. However, caregivers swiftly referred the baby to Chikwawa District Hospital’s neonatal intensive care unit, about 35 kilometres away, because he could not cry, breastfeed or breathe properly.
“I was afraid of losing the baby, who was named after his grandfather, but caregivers constantly check on him and brief me about his condition. He is getting better and I cannot wait to take the baby home,” she said after spending 10 days at the hospital.
The mother, who dreamed of becoming a doctor, wants her baby to make the dream a reality and treat patients with a smile like those who served her in the 14- bed neonatal intensive care unit.
The feedback fills caregivers with joy.
“I’m happy when a little one gets better. When we lose a baby, it feels like I did not do enough. The neonatal audits help my team understand what we could have done better,” says clinician Sharrock Msukwa, checking on the babies in the emergency room.





